Perioperative Care of People Living with Frailty
Bringing together the multidisciplinary team to improve care for people living with frailty
The Centre for Perioperative Care, working in collaboration with the British Geriatrics Society, has now published guidance for the care of people living with frailty undergoing elective and emergency surgery that encompasses the whole perioperative pathway
Frailty is a condition characterised by loss of biological reserve, failure of physiological mechanisms and vulnerability to a range of adverse outcomes including increased risk of morbidity, mortality and loss of independence in the perioperative period. With the increasing recognition of the prevalence of frailty in the surgical population and the impact on postoperative outcomes, The Centre for Perioperative Care (CPOC) and the British Geriatrics Society (BGS) have worked together to develop a whole pathway guideline on perioperative care for people living with frailty undergoing elective and emergency surgery.
Delivering whole pathway, quality perioperative care requires multicomponent intervention, with integration across community, primary, secondary and social care. A multidisciplinary ‘one-team’ approach across these sectors is necessary to deliver each component of the pathway:
- patient and carer involvement, education and empowerment
- preoperative risk assessment and optimisation of physiological status, comorbidities and geriatric syndromes including frailty
- lifestyle modification to improve both perioperative and long-term health outcomes
- shared decision making (SDM)
- optimal intraoperative surgical and anaesthetic management
- quality postoperative care in the most appropriate setting to include rehabilitation
- proactive discharge planning
- links and referral to relevant community, primary care and follow up services
The scope of this guideline covers all aspects of perioperative care relevant to adults living with frailty undergoing elective and emergency surgery. It is written for healthcare professionals involved in delivering care throughout the pathway, as well as for patients and their carers, managers and commissioners. Implementation of the guideline will require collaboration across the four nations of the United Kingdom between all stakeholders, underpinned by an implementation strategy, workforce development with supporting education and training resources and evaluation through refinement of current national audit tools. We believe this is an important step in improving outcomes for our patients and healthcare services.
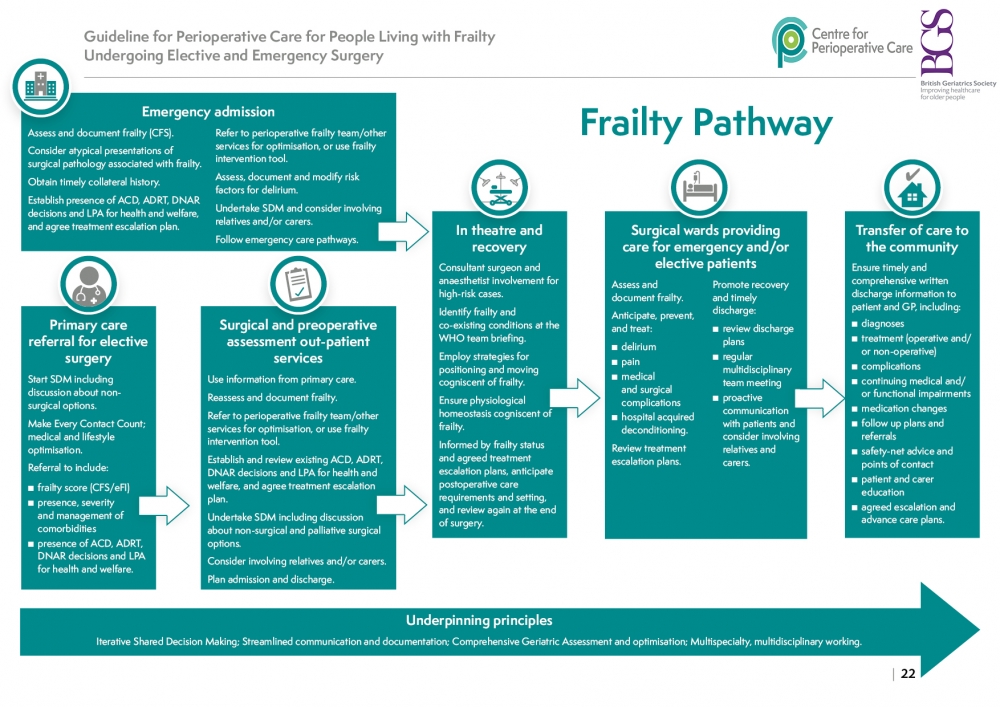
Structure of the Guidance
Perioperative care for people living with frailty is particularly complex and deficiencies in current perioperative pathways have been well described. Despite published interventions for frailty, an implementation gap between recommended care and routine perioperative practice exists. This may be a consequence of too few geriatricians, silo working and difficulties in embedding complex interventions for frailty in the clinical setting, compounded by unintended consequences of time-based targets (for example the 62 day cancer pathway) and a lack of commissioning incentives to embed a whole pathway perioperative team. To address this challenge, this new guideline has been coordinated by CPOC and the BGS, working with patient representatives and all stakeholders involved in the perioperative care of patients with frailty undergoing surgery.
-
Standards
-
Recommendations for people living with frailty and their carers
-
Recommendations for commissioners and providers of surgical services for people living with frailty
-
Recommendations for primary care teams
-
Recommendations for staff working in surgical outpatients and preoperative assessment services
-
Recommendations for staff working in surgical wards providing care for emergency and/or elective surgical patients
-
Specific considerations in the emergency setting
-
Recommendations for staff in theatre and recovery
-
Recommendations for transfer of care to the community
-
Recommendations for quality improvement and metrics
-
Recommendations for Research
We hope that this jointly produced guideline will empower patients living with frailty to work with health care professionals using shared decision making to ensure they receive the best possible care. This is particularly timely as health care services recover after the COIVD pandemic.
Guideline Working Group
|
Organisation |
Name |
|
Association of Palliative Medicine |
Amy Proffitt |
|
Association Surgeons Great Britain and Ireland (ASGBI) |
Lyndsay Pearce |
|
British Dietetic Association (Older People Specialist Group) |
Vittoria Romano |
|
British Geriatrics Society (BGS) |
Jude Partridge |
|
British Geriatrics Society Representative to the Professional Records Standards Body (PRSB) |
Emma Vardy |
|
British Geriatrics Society, Wales |
Nia Humphry |
|
British Orthopaedic Association (BOA) |
William Eardley |
|
Centre for Perioperative Care (CPOC) |
Jugdeep Dhesi |
|
Centre for Perioperative Care (CPOC) |
Louise Bates |
|
Centre for Perioperative Care (CPOC) |
Scarlett McNally |
|
Chartered Society of Physiotherapy (CSP) |
Alison Cowley |
|
College of Operating Department Practitioners (CODP) |
Bill Kilvington |
|
Faculty of Intensive Care Medicine (FICM) |
Daniele Bryden |
|
Getting it Right First Time (GIRFT) |
Adrian Hopper |
|
NHS Elect, Specialised Clinical Frailty Network |
Catherine Meilak |
|
NHS Scotland |
David McDonald |
|
Patient Representative |
Lawrence Mudford |
|
Preoperative Association (POA) |
Ali Curtis |
|
Preoperative Association (POA) |
Shelley Rose |
|
Royal College of Anaesthetists England (RCoA) |
Sarah Hare |
|
Royal College of Anaesthetists Wales (RCoA) |
Tessa Bailey |
|
Royal College of Anaesthetists, Northern Ireland (RCoA) |
Claire Barker |
|
Royal College of Anaesthetists, Scotland (RCoA) |
Laura McGarrity |
|
Royal College of Emergency Medicine (RCEM) |
Eleanor Syddall |
|
Royal College of General Practitioners Scotland (RCGP) |
David Shackles |
|
Royal College of Nursing (RCN) |
Angeline Price |
|
Royal College of Nursing (RCN) |
Beck Diedo |
|
Royal College of Occupational Therapy (RCoT) |
Catherina Nolan |
|
Royal College of Surgeons of England (RCSEng) |
Nicholas Peter Lees |
|
Royal College Physicians (RCP) |
Jane Youde |
|
Specialised Clinical Frailty Network (SCFN) |
Simon Conroy |
|
Trainee Representative, Clinical Quality Commission (CQC) |
Kate Kanga |
|
United Kingdom Clinical Pharmacy Association (UKCPA) |
Sarah Carter |
|
United Kingdom Clinical Pharmacy Association (UKCPA) |
Sarah Tinsley |
|
United Kingdom Clinical Pharmacy Association (UKCPA) |
Derek Taylor |
|
University of Leeds & Bradford Teaching Hospitals NHS Foundation Trust |
Andy Clegg |
|
Vascular Society (VASGBI) |
Rachel Bell |

Jugdeep Dhesi is a Consultant Geriatrician at Guy’s and St Thomas’ NHS Foundation Trust in London. She is clinical lead for the award winning Perioperative medicine for Older People undergoing Surgery (POPS) service, Vice President at the British Geriatrics Society and President of Age Anaesthesia Association. She has led the development of novel education and training programmes for medical and allied health professionals and established a research programme in perioperative medicine. All of this work focusses on improving quality of care for the high risk surgical population, through fostering a collaborative and proactive approach working with patients, their carers, healthcare professionals, managers and policymakers.

Jude Partridge is a geriatrician working in the Proactive care of Older People undergoing Surgery (POPS) team at Guy’s and St Thomas’ NHS Foundation Trust, London. She has a full time clinical role with one session allowing her to continue her research interests.


